   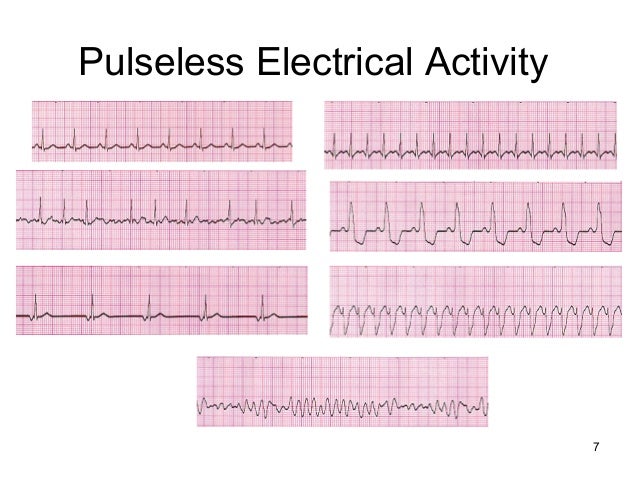 
For example, the identification of true PEA (cardiac standstill) could predict the failure of resuscitation and help inform the decision to terminate CPR, which allows for hospi tal resources to be utilized elsewhere.Understanding the patient’s prognosis will help guide the decision of terminating resuscitation efforts. Pseudo PEA is associated with higher rate of ROSC and survival to hospital discharge.Clinical significance: “Why differentiating True PEA from Pseudo PEA is clinically important” ?.PREM = Pulseless with a Rhythm with Echocardiographic Motion = Pseudo-PEA.PRES = Pulseless with a Rhythm with Echocardiographic Standstill = True PEA.Scott Weingart has suggested another lexicon because of ambiguity around definition of Pseudo PEA: Pseudo-PEA: Presence of cardiac contrac tions (on echo) OR detectable arterial pulsation by POCUS pulse check *.Pulses are truly absent (no arterial pulsation on POCUS pulse check) *. True PEA: There are no cardiac contractions (cardiac standstill), hence there’s no cardiac output and blood flow.Previously these two conditions were lumped together as they share presence of cardiac electrical activity on ECG monitor and undetectable pulses by manual technique *.Only 15% of participants could accurately assess for the presence of a pulse within 10 seconds and only 2% identified pulselessness correctly within 10 sec *. In a study assessing the diagnostic accuracy of first responders of detecting a manual pulse in patient with and without a true pulse, the sensitivity for pulselessness approached 90%, however the specificity was only 55%.Since this differentiation hinges on presence or absence of a pulse, it’s worth mentioning here that the palpation technique is poor at determining whether or not a patient has a pulse.Patients with pulse pressures were designated as having “pseudo-PEA” and those without, as having “true PEA” *. In a study published in 1992 among patients with apparent PEA, a group of patients found to have aortic pulse pressure waveform using arterial line.However not all PEA meet cardiac arrest by definition. bradycardia, normal sinus rhythm, etc.) and no palpable pulse. The diagnosis of PEA is based on a patient having an organized, non-shockable rhythm (e.g. Rarely patients with VT may presents with extreme instability (but not in cardiac arrest).Rhythm: Any organized rhythm (even including VT).Extreme tachycardia, terminal bradycardia (e.g.Dependin g on the underlying cause and severity of the disease, these patients may deteriorate to full-blown cardiac arrest within a couple of minutes.The center of focus in this post is pulseless electrical activity (PEA). Non-shockable rhythm (asystole and pulseless electrical activity).ventricular fibrillation “VF” ploymorphic ventricular tachycardia “pMVT”, VT) or Rhythm: Generally, initial rhythm in cardiac arrest could be:.A brief generalized seizure or myoclonic jerks may be the initial manifestation of cardiac arrest, which can confuse the lay provider and delay the application of lifesaving BLS care.deep, slow breaths at a rate of 1-2/min) or gasping may be present immediately after the collapse, which can delay the recognition of cardiac arrest. Unresponsiveness, absence of spontaneous breathing and no palpable pulses.It is the final common pathway of all life-threatening conditions and is referred to the sudden cessation of “mechanical” cardiac activity (pump failure), as confirmed by the absence of circulation.A directed therapeutic approach to go along with aggressive resuscitation will provide patients with Pseudo PEA the best chance to survive. It is imperative for physicians to be able to distinguish pseudo-PEA from true PEA as the prognosis and man agement of these patients differ. Therefore lumping together all patients with pulseless electrical activity and treating them according to current ACLS guidelines is not appropriate. However PEA is a spectrum of disease and not all cases of PEA are in cardiac arrest state. The overall survival rate of patients with PEA is much worse than that of cardiac arrest patients with shockable rhythms. Patients with pulseless electrical activity (PEA) account for up to 30% of cardiac arrest victims. Point-of-care ultrasound in cardiac arrest.Return of spontaneous circulation (ROSC). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
